Chronic pain is classified as a pain or discomfort that is ongoing and lasts three months or longer. It is typically caused by an underlying chronic condition, although not always. Unlike pain from pulling a muscle or stubbing your toe that goes away after the injury is healed, chronic pain can last years if not managed by a physician.
This type of pain is not always constant, but it does disrupt daily life by preventing patients from doing what they love.

Things to Know About Chronic Pain
What Causes Chronic Pain
For many people, chronic pain begins after an injury or trauma. Other times, it can begin without an obvious cause. Some of the most common causes of chronic pain are:
-
- Previous surgeries or injuries – Old injuries can cause nerve damage because they either were not treated properly the first time or they healed incorrectly.
- Back problems – There are a variety of back conditions that contribute to chronic pain, such as SI Joint Pain, herniated discs, deterioration of the spinal column, spinal cord compression, and many others.
- Migraines or other types of headaches – While chronic headaches are difficult to diagnose, common causes are inflammation, blood pressure issues, stress, or hormone changes in women.
- Arthritis – Arthritis is one of the most common causes of chronic pain and can cause limb deformities, loss of range of motion, stiffness, and inflammation.
- Nerve damage – An injury, accident, or infection can cause chronic nerve pain (neuropathic pain). When nerves are damaged, they are unable to function properly and that oftentimes leads in a loss of communication between body parts and the brain.
- Fibromyalgia – Fibromyalgia is a musculoskeletal condition that causes widespread muscle pain throughout the body. Studies show that this condition worsens pain by affecting the way your brain processes these signals.
How Does Chronic Pain Affect My Body?
When pain is experienced for a long amount of time, your nociceptors go into overdrive and become more sensitive to pain. They produce lower level signals, making you feel more pain than you are actually experiencing. This is problematic because your body is likely not harmed, but your pain receptors exaggerate the pain.
When an injury or trauma occurs, the area’s pain sensors (nociceptors) are “turned on.” They send an electrical current that travels along the nervous system until it reaches the brain. Your brain understands that signal and sends the message that you are hurt. In chronic pain patients, the nerves continue sending the pain signals to the brain, even after the injury is healed.
Why Are Narcotics Bad for Chronic Pain?
Narcotics, in chronic pain patients, create a cyclical relationship and dependency. At first, these drugs may relieve pain by attaching themselves to your brain’s endorphin receptors. However, after any length of time, the receptors become dependent on the medication’s effect. The brain limits the amount of endorphins it produces, reducing the body’s natural painkillers. Without natural endorphins, narcotics have to be taken to maintain a level of comfort.
This causes problems when the patient is no longer prescribed these medications from a physician, because their body has become dependent on the narcotics’ effect on the brain. Your brain and body need that chemical to function regularly. Stopping or lowering the dose can cause your body to react poorly, including nausea, shakes, headaches, and other serious problems.
Available Treatment Options
Treatment for chronic pain will depend on your pain’s severity and your physician’s diagnosis. The root cause of the pain will also determine the treatment plan your physician designs.
Medications for Chronic Pain
Medication can be helpful to patients who suffer from chronic pain. Over-the-counter pain relievers such as acetaminophen (Tylenol) or NSAIDs like aspirin and ibuprofen are useful in reducing inflammation and stiffness that worsens chronic pain.
Physicians do not recommend opioids due to the aforementioned risk of dependency and danger of abuse.
Analgesics such as antidepressants and anticonvulsants are useful in chronic pain that is caused by nerve-related disorders. This includes pinched nerves, sciatica, and herniated discs.
Procedures for Chronic Pain
If the chronic pain worsens and other pain relief methods have not been successful, your physician may recommend a medical procedure.
Some examples include:
- Electrical stimulation
- Nerve block injections
- Acupuncture
- Facet joint injection
- DRG therapy
- Spinal cord stimulation
There is no cure for chronic pain, but when managed effectively, patients can live their lives relatively pain-free and comfortably.
Under a pain management specialists’ supervision, it is recommended that patients who are looking to reduce chronic pain make lifestyle changes in order to promote health and wellbeing. This includes being active, incorporating low-impact cardio into their daily routine, eating a healthy diet, and getting enough sleep.
Learn more about pain management and how the team at Progressive Pain Management work with their patients to create a personalized pain management plan that works best with their lifestyle and needs.
Fill out the form below to get started today.
Muscle pain affects anyone, including powerlifters, construction workers, and pregnant women. Failure to address the issue leads to chronic pain, affecting how one moves. This condition occurs when muscle fibers get stuck in contraction, forming bumps known as trigger points.
Massages and chiropractic adjustments can help relieve the pain. However, trigger point injections may be necessary to eliminate chronic muscle pain.
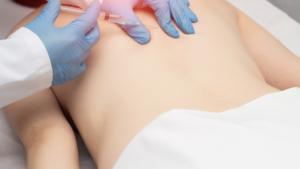
Trigger Point Injections for Treating Chronic pain
What Are Trigger Point Injections?
Trigger point injections involve injecting a local anesthetic into contracted muscles to relax them and relieve pain. The affected muscles often form bumps under the skin that cause tenderness due to restricted blood flow.
Trigger point injections effectively relieve the symptoms of myofascial pain syndrome, a condition that affects the muscles and the tissue surrounding them. Trigger points can form due to the following reasons:
- Musculoskeletal disorders
- Lack of regular exercise
- Vitamin deficiency
- Prolonged poor posture
Trigger point injections can include a combination of local anesthetic and steroids that block pain receptors and reduce muscle inflammation and knotting.
The Benefits & Conditions They Treat
Trigger point injections can help relieve chronic pain affecting the muscle and nervous system. Some of the conditions treatable with the injections include:
Migraines
Trigger points in the neck and shoulder muscles may cause tension headaches which can be mild or severe and throbbing. Trigger point injections can help deliver immediate relief to patients suffering from severe headaches or frequent migraine attacks.
Myofascial Pain Syndrome
Myofascial pain syndrome is a chronic condition that affects muscles, causing them to knot and send painful sensations to unrelated regions. Several causes, such as injury, poor posture, and psychological stress, cause muscle stiffness and limit motion.
Trigger point injections can help block neural pathways and relieve pressure from the contracted muscles. The injections can also help torn muscles heal.
Fibromyalgia
Fibromyalgia is a chronic pain condition whose symptoms include widespread body pain and fatigue. Patients also experience mental distress and trouble sleeping.
Injecting an anesthetic into a trigger point can help deliver relief from the pain and relax any knotted muscles.
What Happens During The Procedure?
Trigger point injections typically take minutes and require a brief in-office appointment. Injecting trigger points may be painful, but this is a great sign your doctor is treating the correct spot.
During the procedure, your doctors will first identify your trigger point. After sterilizing the area of concern, they will inject the trigger point with local anesthesia to relax the muscle and bring relief. The dry-needle technique is used for patients allergic to anesthesia.
Trigger Point Injections with Our Team of Experts
Trigger Point Injection is effective in providing relief to patients experiencing chronic pain. The injections help the inflamed muscles relax, allowing the blood vessels to function freely.
Our team of experts at Progressive Pain Management focuses on interventional pain procedures that bring relief to patients with chronic pain. Our physicians have the expertise to administer some of the most advanced pain management techniques. Please fill out our form and let us help you manage your chronic pain.
Chronic pain is pain that is ongoing or lasts longer than 6 months. And while this pain can be debilitating and affect your daily life, it can also cause other serious health issues and affect the central nervous system.
How Pain Signals Work in Your Body
Your brain and spinal cord work together to receive pain signals from nerves and muscles, which send patterns of signals to the rest of the body. These signals help the body control leg, arm, and spine movements. These signal patterns develop and allow us to ride bikes, walk, or even play an instrument or knit.
However, when you are experiencing chronic pain, the sensors and nerves that send out pain signals “misfire” and the brain and spinal cord are unable to function properly in accordance with what the signal is trying to communicate. The spinal cord reacts in a way that increases a normally harmless pain signal, creating severe chronic pain.
How Chronic Pain Affects the Central Nervous System
The Relationship Between Pain and the Central Nervous System
When the spinal cord increases the pain signals, your central nervous system understands them as incredibly intense and painful. Even harmless signals are miscommunicated as horrible pain signals. The central nervous system operates differently than a pain-free nervous system and causes the patient to become more sensitive with less provocation. This is referred to as “central sensitization.”
Not only are patients who suffer from central sensitization extremely sensitive to things that should hurt, but ordinary things like a simple touch or slight pressure can be excruciating. Pain that typical patients may describe as a two on a numeric pain scale (1-10 level of pain) may feel like an 8 or a 9 for patients that have central sensitization. The pain becomes extremely amplified, even doing activities such as doing the dishes or walking to the mailbox.
Central Sensitization
Central sensitization is a condition that is associated with the maintenance of chronic pain. During flare ups, the nervous system goes into shock and is in a constant state of high reactivity. Being highly reactive lowers the threshold for the cause of pain and the ability to maintain pain after the injury is healed.
Central Pain Syndrome
Central pain syndrome is a neurological condition. It is caused by a dysfunction that affects the central nervous system, such as multiple sclerosis, Parkinson’s disease, or spinal cord injuries. It can take months or even years after an injury or trauma to affect the CNS.
Similar to central sensitization, central pain syndrome is heightened by light touch. However, the most common symptom is the sensation of burning. Pain increases when the temperature drops, and a loss of sensation may occur.
How Central Sensitization Affects Pain
As peripheral pain signals are transmitted to the spinal cord, there are receptors that determine whether or not the spinal cord should respond. Weak muscle signals can be amplified and misinterpreted as pain. The spinal cord becomes highly irritated and misreads the signals from parts of the body, making them stronger than usual. Patients have even experienced intense pain from the weight of a blanket or bed sheet.
This is the central amplification of a peripheral pain signal. The peripheral and central nervous systems work together to help the body determine how the body reacts to a sensation.
Overtime, chronic pain and misread signals can physically change the way the central nervous system responds to pain. The experts at Progressive Pain Management can help control your chronic pain and reduce symptoms caused by central sensitization.
Fill out the form below to talk to our doctors about chronic pain and symptoms you may be experiencing.
Facet joints are small, bony joints that sit along the spine. They are paired up from the neck to the lower back area. When the joints get inflamed, they cause pain that can be severe. The pain can be acute or chronic, caused by a variety of conditions.
The pain radiates to other parts of the body and causes indirect pain. For pain that starts in the lower back, it’s common for the pain to move to the thighs and buttocks. If the pain starts in the neck or upper back region, it can transfer to the shoulders, and arms, and even cause headaches.
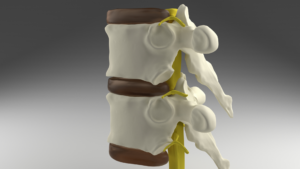
Facet Joint Injections for Chronic Pain
What is a Facet Joint Injection?
The injection is a strong anti-inflammatory steroid that gets inserted into the facet joint. The medication is a mixture of a local anesthetic and a steroid, similar to a cortisone injection. Before performing the injection, your doctor will explain the procedure, have you sign all the appropriate consent forms, and then have you lie on your stomach.
The procedure is minimally invasive. X-ray guidance is used to locate the facet joints and helps guide the needle to the exact location. The actual injection only takes a few minutes, but you may want to allow for additional recovery time depending on the type of anesthetic you choose. Some doctors will let you choose a local anesthetic or a stronger general anesthetic. The general anesthetic may cause drowsiness and sedation will take longer to wear off.
What to Expect After the Injection?
Right after the injection, you will feel relief from pain. That is due to the anesthetic in the injection, and only lasts for a few hours. The injection site may become sore after a few days, and the pain is not uncommon to resume the day after the injection. About 1-2 days after the injection, the medication will begin to take effect and help reduce your pain on a daily basis.
It is advised to take it easy following the injection and only to resume normal activity when it is comfortable to do so. Your doctor may recommend applying ice to the injection site. This will help reduce any swelling and soreness following the procedure.
How Long Does a Facet Joint Injection Last?
Immediately following the injection, you may feel lessened pain. However, this is temporary relief until the medication kicks in. That can take between 2-7 days after the injection.
If the first injection is successful in managing your pain, your doctor may perform additional injections. The amount of relief depends on your specific pain and because there are a variety of pain receptors in the spine, the long-term effect of these injections cannot be predicted. Everyone’s pain is different, so the treatment effectiveness will vary.
There are very few risks associated with this type of injection. The most common being tenderness and pain at the injection site, although this is temporary. Side effects of steroids may include weight gain, water retention, and temporary increase in blood sugar.
Facet joint injections are an excellent alternative to undergoing serious back surgery. Talk with your doctor today to discuss your options for getting relief from your pain and taking one step closer to bettering your quality of life.
Risks Associated with the Facet Joint Injection Procedure
As with any type of injection or invasive procedure, there are certain risks or complications that could arise:
- Allergies: In most cases, the allergic reaction is caused by the X-ray contrast or steroid, not the local anesthetic. Severe allergies are rare.
- Bleeding: In patients who are taking blood thinners or have a bleeding disorder, it is possible to have some bleeding as a result of the injection.
- Discomfort at the Injection Site: Worsened pain or discomfort at the injection site. Long-term pain is uncommon.
- Infection: Minor infections occur in less than 2% of facet joint injections. More complex infections are rare, only happening in 0.1% of injections.
Fill out the form below to contact the Progressive Pain Management team and learn more about facet joint injections.

