Often, a group of nerves – called a plexus or ganglion – causes pain to an area of the body. This pain can be “turned off” by using a specific injection that blocks the pain signals from reaching the brain. This is called a nerve block.
Nerve block injections are used to treat chronic pain when medications or other treatments prove to be ineffective or cause negative side effects. They allow a damaged nerve proper time to heal, provide temporary pain relief, and can be used to identify a specific cause of pain. Oftentimes, your physician will perform a test block with a local anesthetic. If you have positive results and pain relief from the test block, your doctor will move forward with an injectable nerve block.
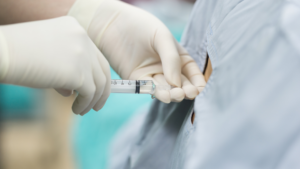
Nerve Block Injections for Treating Chronic Pain
Why are Nerve Block Injections Used?
Nerve block injections are used for a variety of purposes. Patients who suffer from acute or chronic pain may receive a nerve block injection for temporary pain relief. Since pain is such an individual experience, nerve blocks are also used to help physicians diagnose the source of pain by measuring the patient’s response to the injection. This is helpful to determine a treatment plan.
Other purposes for nerve blocks are:
- To predict the outcome of any given treatment. Prognostic nerve blocks are performed to determine if a more permanent treatment (surgery) would be more successful in treating pain.
- To avoid surgery, in some cases.
- To prevent additional pain from a procedure or surgery that can cause negative side effects, such as phantom limb pain.
Types of Nerve Blocks
Since nerve block injections can be used for a variety of purposes to help reduce, treat, and prevent pain, it is no surprise that there are many different types of nerve blocks.
The benefit of nerve blocks is that they can be used in almost every area of the body to treat pain. Because of this, there are different nerve block types. Notype of pain should be treated equally. Here are few types of nerve blocks that are available and why they may be utilized in your pain management treatments:
- Therapeutic nerve block: This type of nerve block contains a local anesthetic to control acute pain.
- Prognostic nerve blocks: These are used to help your physician predict the effectiveness and outcome of a given treatment.
- Diagnostic nerve block: This block contains an anesthetic that helps relieve pain and helps pain specialists determine the root cause of chronic or acute pain.
- Sympathetic nerve block: This type of block is used to determine if there is any type of damage or injury to the sympathetic nerve chain – the network of nerves that extends the length of the spine.
- Preemptive nerve blocks: These types of nerve blocks are meant to prevent pain after a surgery that can cause issues like phantom limb pain.
How are Nerve Blocks Performed?
Nerve block injections use imaging guidance – such as fluoroscopy or CT scans – to guide the needle into the injection site. This allows the physician to place the needle in the most accurate location for the injection to be most beneficial. The syringe will be filled with medication, depending on what the patient needs.
A small needle will be inserted through the skin and directed towards the injection site. A small amount of contrast material may be used to confirm needle placement in the appropriate location. The injection itself will be administered with a syringe much like one that would be used for a routine vaccination. The doctor will fill the syringe from a small vial of medication. The type of medication used depends on individual patient needs.
This is typically performed as an outpatient procedure and only takes a few minutes to administer.
Your physician will position you on the table or surface to allow access to the site to be injected. Using imaging guidance, the doctor will identify where the needle needs to be placed. In some cases, more than one injection may be required, depending on the area of pain that needs to be covered. The medication will go into effect rather quickly, but the doctor will have you stay in the office to ensure no immediate and unexpected side effects.
Side Effects and Risks of Nerve Block Injections
Nerve blocks are safe; however, like any procedure and injection, there is always a risk involved. Typically, nerve blocks carry fewer side effects than other types of medication.
Some side effects include:
- Infection
- Bleeding
- Injection site soreness and tenderness
- Bruising
- Damage to nerves
- Elevated blood sugar
- Horner’s syndrome
Nerve blocks provide temporary relief from pain; the results can vary from patient to patient. Speak to your doctor about your options when it comes to relieving your pain so you can determine a course of action. Nerve blocks are among a variety of anesthetics used to treat pain caused by a group of nerves.
Contact Progressive Pain Management to learn more about nerve block injections and how they can help combat your chronic pain. Fill out the form below.
Complex regional pain syndrome (CRPS) is a chronic pain condition that typically affects a limb, like a leg or an arm. Damage or malfunction to the central nervous system is what is believed to cause complex regional pain syndrome. The central nervous system contains the brain and spinal cord. Things like injuries, surgeries, strokes, or heart attacks are common causes.
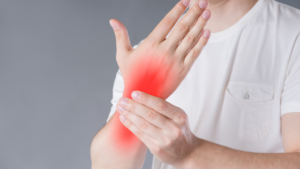
What is Complex Regional Pain Syndrome
This condition is not common. In fact, it is difficult to diagnose and is historically tricky to treat. The affected area is not only extremely painful but other symptoms can include a change of body temperature, discoloration, and swelling in the affected area.
CPRS can be divided into two types: CRPS-I and CRPS-II. CRPS-I is previously known as reflex sympathetic dystrophy (RSD) syndrome. This type is when patients do not have a confirmed nerve injury or disorder. CRPS-II (also known as causalgia) is when the condition stems from a confirmed nerve injury. Despite there being two types of CRPS, treatments are similar.
Symptoms of Complex Regional Pain Syndrome
The symptoms of CRPS vary. The main symptom that is present is long-term severe pain that may be constant. This pain is often described as burning or a pins-and-needles sensation. Symptoms may change over time, but pain, swelling, redness, and hypersensitivity (allodynia) are typically the first symptoms that occur. Pain has been known to spread, even if the affected area is only a hand or even finger. While this is rare, complex regional pain syndrome may spread to other extremities, such as the opposite limb or other area of the body.
Symptoms can go away on their own, overtime.
Other symptoms of CRPS include:
- Changes in hair growth patterns
- Joint stiffness
- Decreased muscle coordination
- Abnormal sweating pattern in the affected area
- Tremors or jerking of the affected limb
Diagnosis and Treatment Options
Diagnosis
CRPS is diagnosed based on a patient’s medical history and present symptoms. It is especially difficult to diagnose because the symptoms are common to other conditions as well. As a person’s symptoms improve, it is even more difficult to diagnose.
Certain tests are used to rule out other disorders and conditions that display similar symptoms, such as arthritis, Lyme disease, a clotted vein, or a general muscle disease. These tests can provide your physician with clues about what is causing your pain. A careful examination should be performed to determine if an injury is the root cause of the pain – the key feature to CRPS. Thorough examinations help assess the pain and determine if other treatable conditions are present and not ignored.
Imaging tests such as magnetic resonance imaging or triple-phase bone scans may be used to confirm a diagnosis. CRPS is often related to a process where certain cells break down bone and release calcium into the blood. However, this symptom can be caused by other diseases as well. X-Rays are used to show a loss of minerals from your bones. This is common in later phases of the disease. Sympathetic nervous systems tests look for disturbances in your sympathetic nervous system by using thermography to measure your skin temperature and blood flow. Other tests can measure the amount of sweat on your limbs. Irregular results can lead to an accurate prognosis of complex regional pain syndrome.
Treatment Options
The goal of treatments is to lower the intensity of pain and reduce muscle spasms. Your physician may recommend different types of treatment options depending on the severity of your pain and symptoms you experience.
Therapies include:
- Physical Therapy: Physical therapy is used to keep the painful body part moving to increase blood flow. Exercise helps increase flexibility, builds strength, and improves the function of the affected area.
- Nerve Blocks: Sympathetic nerve blocks can provide temporary relief from pain, but does not have any long-term benefits. Nerve blocks involve injecting an anesthetic next to the spine to block the nerves from communicating pain signals with the brain.
- Medications: Various medications are used to help reduce pain. Your doctor may recommend over-the-counter pain relievers such as Naproxen, Ibuprofen, or Aspirin. If a patient is suffering from neuropathic pain, antidepressants may be prescribed. Corticosteroids, such as prednisone, are used to reduce inflammation and improve mobility.
- Heat Therapy: Applying heat may reduce swelling and discomfort on skin that has varying temperatures.
- Biofeedback: Biofeedback techniques help you become more aware of your body so you can train it to relax and reduce pain. This involved being hooked up to an electrical sensors that measure your bodily functions like heart rate. This information helps train your mind and body to understand your pain on a deeper level.
Contact Progressive Pain Management to learn more about complex regional pain syndrome treatment options. Fill out the form below to get started.
Anyone with stiff joints or chronic pain knows how relaxing it can be to slip into a warm bath at the end of the day. This is because the water pressure alleviates the pressure you place on your joints. There is a lot of science behind this buoyant force, and it is the same reason why you feel weightless in water.
When you live with chronic pain, you know that any relief is welcomed. Many pain specialists and physical therapists recommend water therapy for patients with fibromyalgia, osteoarthritis, or chronic joint pain. This does not always mean participating in group water aerobics. Aquatic therapy can also include floating therapy and water yoga.

Aquatic Therapy to Help Reduce Pain
How Aquatic Therapy Helps Ease Chronic Pain
- Water Aerobics for Osteoarthritis
People with osteoporosis benefit greatly from doing water exercises. This allows their muscles to stretch and strengthen using the gentle resistance of water. Stretches like lifting your knees to your chest and using the side of the pool to do leg lifts and arm stretches are good for your muscles and improve your range of motion.
Water aerobics are another type of therapy that prove beneficial for patients with osteoarthritis. Walking in the water, water jogging, and other movements that make your hip joints more limber build strength without having to exercise on a treadmill.
- Floating Therapy
The most simple type of aquatic therapy is floating therapy. This is to simply float. This can be done floating vertically, so that your body is deeply emerged in water. This lets the water pressure have a more therapeutic benefit – the deeper you go, the stronger the pressure. Floating can lower your blood pressure and improve neurological conditions.
Another type of floating that has profound neurological benefits and can aid in relaxation therapy is floating in a super Epsom salt bath. This is a shallow, high-buoyancy tub that focuses on sensory deprivation. Sensory deprivation is a relaxation technique that helps eliminate external stimuli that affects pain.
- Hot Tub Therapy
Patients with back pain regularly find relief from their pain when heat is applied. A take on heat therapy, hot tub therapy combines relaxation from aquatic therapy and the warmth of heat therapy. This also helps patients with osteoarthritis and fibromyalgia. The warm, bubbly water lessens joint stiffness and pain. It also boosts blood flow to the affected area.
Be sure to follow your physician’s recommendations regarding hot tub therapy. The heat can occasionally cause headaches or dizziness, so always follow healthy hot tub regulations.
- Water Yoga
Just like on dry ground, doing water yoga is a well-known rehabilitation technique for patients with chronic pain. However, water yoga adds in a natural resistance. Water pressure encourages deeper, diaphragmatic breathing which is important to the practice of yoga. Yoga is good at preventing muscle soreness, reducing low back pain, and improving neurological conditions. Many yoga stretches are more comfortable when you have the water pressure working against you instead of gravity. It can be easier to sustain the poses and make the poses more effective.
Living with chronic pain is uncomfortable and can prevent you from doing what you love. Easing the symptoms with aquatic therapy can help, but getting the right kind of help from a qualified physician is best. Contact the team at Progressive Pain Management today using the form below.
After surgery, pain is natural. Managing and controlling that pain is crucial to your healing and recovery. More than 80% of patients report pain after surgery. While you should expect some pain after surgery, your physician will take proper precautions and every effort to lessen your pain.
Managing pain after surgery is the most effective way to ensure a healthy recovery. Having a postoperative treatment plan may help reduce the risk of developing complications. When your pain is properly managed, your quality of life will be restored, and essential tasks like walking can be resumed normally.
Post-Surgical Pain Care
Pain after surgery may surprise you. Oftentimes, the painful area is not where the surgery was performed, but instead, referred pain. This means the pain is experienced somewhere other than the affected area. Referred pain occurs because of how pain signals travel along you nerves.

The Importance of Post-Surgical Pain Care
Other types of pain you may experience after surgery are:
- Muscle Pain: Lying in a chair or operating table can result in pain in your neck, shoulders, back, or chest.
- Throat Pain: After surgery, you may experience scratchiness or dryness in your throat. This can make it sore and uncomfortable.
- Movement Pain: Moving and performing important tasks like sitting, walking, and even basic movements like arms and feet can cause pain at or around the incision site or affected area.
Treatment Options for Pain Relief
The goal of pain management after surgery is to relieve an uncomfortable, painful experience and to control pain. However, when there is postoperative pain, you might think the surgery was a failure. Pain after major surgery is to be expected. Your doctor will work with you to determine the best course of action and an effective treatment plan.
Nerve Blocks
Your doctor may recommend a nerve block to control your pain after surgery. Nerve blocks are minimally invasive injections that block pain signals from reaching your brain. This type of treatment helps cut down on the amount of pain medication you will need to take.
Over-the-Counter Pain Medication
Your doctor will likely order over-the-counter pain medications to help relieve your pain after surgery. These medications often include anti-inflammatory medications such as Advil and pain relievers like Tylenol. Over-the-counter medications have minor side effects, if any at all, and are safe to take without the risk of forming an addictive habit. Be sure to follow your doctor’s instructions
At-Home Techniques
There are a number of at-home techniques designed to help relieve pain during recovery.
- Relaxation Techniques: Listening to calming music, biofeedback, and meditation a few of the ways you can relieve your pain at home. Learning to focus your attention on something other than your pain is a natural way to lessen your pain.
- Heat & Cold Therapy: This is an option to reduce swelling and control your pain at home. Your doctor will advise you on how to do this at home. Sometimes only heat, only cold, or an alternating method of both can be effective.
- Exercise: As your healing permits, slowly incorporating low-impact cardio and strength-training exercises help your body reduce pain. Exercise releases endorphins which act as your body’s natural opiate, therefore lessening your pain and discomfort. Exercise should only be done once your doctor has cleared you to resume normal activity. Always consult your physician before beginning an exercise routine.
Regardless of how your postoperative pain is managed, make sure you are comfortable with the treatment plan. Keep open lines of communication with your doctor and nurses to address any concerns or issues that may arise. Stress, anxiety, and miscommunication can all make your pain worse and cause a negative healing experience.
Fill out the form below to contact the team at Progressive Pain Management and learn about treatment options for continual care and pain management.
The field of pain management typically deals with traditional methods for evaluating, diagnosing, and treating various types of acute and chronic pain. However, as more research develops and the field of medicine progresses, physicians are able to learn about the complex intricacies of pain. This has led to a sub-specialty called interventional pain management.
What is Interventional Pain Management?
Conventional pain management treatments such as prescription medications, physical therapy, and other non-invasive techniques help reduce pain. What interventional pain management does differently is that it uses injections and radiofrequency to directly address and treat the root cause of your pain.

What is Interventional Pain Management?
Understanding a patient’s pain, the physiology of pain, and available treatments allows pain management specialists to create a multidisciplinary approach that utilizes a variety of techniques best suited to your pain and lifestyle. Interventional pain management has broadened the scope of technology and treatments that are available, effective, and ultimately able to restore your quality of life.
Types of Interventional Pain Management
Injections like nerve blocks, epidural steroid injections, facet joint injections, neuromodulation, and other interventional techniques are used to treat chronic pain disorders with great accuracy and precision.
Physicians oftentimes will use fluoroscopy to perform the injection. This type of X-Ray guidance allows your physician to see exactly where the injection is being placed in the joint to address the source of pain.
Nerve Block
A nerve block is an injection that is directed towards a specific nerve or group of nerve to treat pain. The injection, an anesthetic or anti-inflammatory medication, blocks the pain signal traveling from that location to your brain, quite literally “turning off” the pain you feel. The block decreases inflammation in the affected area.
Epidural Steroid Injection
Epidural steroid injections are another type of nerve block, but they are injected into the epidural space of the spine. The medication calms the nerve, reducing the painful sensations you feel. Epidural steroid injections are used to treat patients with pain caused by a compressed spinal nerve root, sciatica, and even osteoarthritis.
Facet Joint Injections
Facet joints connect the bones of the spine together, allowing for motion and movement. Inflammation causes pain, and facet joint injections can be used to reduce that pain. These injections are placed alongside the joint, and usually involve a concoction of both a steroid and numbing agent. Patients who have not had success with conventional treatments and suffer from neck, arm, low back, or leg pain that is caused by inflammation of the facet joints is a candidate for this procedure.
Radiofrequency Lesioning
Radiofrequency lesioning reduces pain by preventing transmission of pain signals. Radiofrequency utilizes electrical currents to essentially burn small piece of nerve tissue, creating a long-lasting interruption of pain signals to the brain. This is a non-surgical option to reduce chronic pain
Spinal Cord Stimulation
Spinal cord stimulation (SCS) is a type of neuromodulation that helps treat pain that affects the central, peripheral, or autonomic nervous systems by providing electrical stimulation via implanted devices. A small device, similar to that of a pacemaker, is implanted in the back along the spine. The generator transmits low-voltage electrical currents to the spinal cord instead of pain signals. Patients may feel a slight tingling sensation instead of their pain.
Living with chronic pain is not normal, and patients should know that technology is quickly evolving to provide physicians with the most effective and state-of-the-art treatment options for battling chronic pain. Fill out the form below to learn more about how chronic pain can be managed with an interventional pain specialist. The team at Progressive Pain Management is here to help you reduce pain and improve your quality of life.

