Epidural steroid injections (ESI) are a minimally invasive procedure performed to help reduce inflammation and pain caused by nerve root compression. Herniated discs, bone spurs, or spinal stenosis cause nerve compressions. Pain, numbness, or weakness along the nerve are symptoms of nerve compression, referred to as radiculopathy. This pain can last for days or even years if left untreated.
An epidural steroid injection aims to help reduce inflammation along the nerve root. Medication is injected in the fat-filled area between the bone and the protective layer of the spinal nerve, called the epidural space. These injections are intended to reduce pain so that normal activity and a physical therapy program can be resumed.
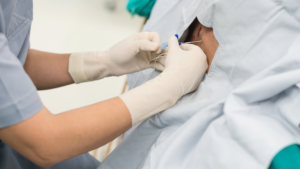
What is an Epidural Steroid Injection
What is an Epidural Steroid Injection?
There are multiple types of steroid injections, most commonly described according to where they are injected. Steroid injections in the neck are called cervical epidural injections. Injections performed in the middle back are thoracic epidural steroid injections, and injections in the lower back are lumbar epidural injections.
The injections can also be labeled according to the direction of the needle. Most epidural steroid injections are placed between the lamina. This is called an interlaminar epidural steroid injection. The needle is aimed upwards toward the head and goes in between two laminae. Another type of injection is a transforaminal steroid injection. The needle travels along the course of a nerve and enters the spine from a diagonal direction. A caudal approach to ESIs allows the needle to enter directly into the epidural space through the sacral hiatus – a small boney opening directly above the tailbone.
The steroid injection contains a corticosteroid, such as triamcinolone, methyl-prednisolone, or dexamethasone, and an anesthetic numbing agent like lidocaine. They are injected into the area between the vertebra and the protective sac surrounding the spinal cord and nerves.
Why Are They Used?
These steroid injections are used in patients who suffer from pain in the neck, arm, lower back, or have sciatica. This treatment has proven beneficial to those with severe inflammatory conditions. Patients who have the following conditions are candidates for epidural steroid injections:
- Spinal Stenosis – a narrowing of the spinal canal and nerve root canal
- Herniated Disc – the material inside a disc can bulge or rupture through a weak area in the cartilage and come in contact with a spinal nerve.
- Degenerative Disc – breakdown or aging of a spinal disc causing the disc space to collapse or growth of bone spurs.
- Sciatica – compression of nerves that causes pain to travel into the buttocks and down the legs.
In some cases, ESI can be used to determine whether surgery will be successful in patients who have a herniated disc. The injections can ease pain enough so a physical therapy routine can be established.
Risks Involved with Epidural Steroid Injections
ESI procedures have been performed for many years and is considered a safe and effective treatment. Although uncommon, some patients do experience side effects from the medication. Patients may experience a “steroid flush” which is a flushing of the face and chest that can be accompanied by a low-grade fever.
Other side effects may include:
- Trouble sleeping
- Temporary water retention
- Anxiety
Serious complications are very rare, but could include an allergic reaction to the contrast dye, infection, nerve damage, or bleeding. When this procedure is performed with fluoroscopic guidance, the risk is minimized. Generally, this type of procedure and injection is very well tolerated by most patients.
To learn more about epidural steroid injections and how they can help back pain, fill out the form below:
Failed back surgery syndrome (FBSS) is the term for a patient’s continued pain after an unsuccessful back surgery. The patient is usually referred to a pain management specialist to treat pain.
The goal of spinal surgery is to decompress a nerve root or to stabilize a painful joint. FBSS occurs when surgery is unsuccessful or negatively affects a structure near the problem area.
Spinal surgery is complicated because it can be hard to diagnose the cause of the pain. X-Rays and MRIs limit what doctors can see because the pain often occurs when the patient is moving and active. Imaging only provides still images.

Failed Back Surgery Syndrome: Signs, Symptoms, and Treatment
Signs & Symptoms of FBSS
One common complaint physicians hear from patients is chronic back pain. However, not everyone experiences the same pain, and the type of pain they experience can vary, based on their spinal disorder, their previous procedure, or underlying cause of FBSS.
Other types of pain that can be associated with FBSS are:
- Nociceptive Pain – Localized pain that may be dull or sharp.
- Neuropathic Pain – Nerve-related pain is caused by nerve or spinal cord damage.
- Radicular Pain – Radicular pain radiates from one area to another
Other common symptoms of Failed Back Surgery Syndrome include:
- Return of original symptoms & pain – When the symptoms return that the original procedure was intended to correct, it may be a sign of FBSS.
- Reduced mobility – Recovering from back surgery is a process. However, if mobility is reduced or limitations arise that are different than predicted by your physician, it could be a sign of FBSS.
- New problems arise – While the surgery may correct the original symptoms, new pain in a different part of the spine should be discussed with your doctor.
- Onset of Headaches – If headaches were not a part of your medical history prior to having surgery, this may be a sign of nerve damage after a spinal procedure.
Diagnosing Failed Back Surgery Syndrome
The first step to diagnosing FBSS pain is to see a doctor for a physical exam. Motion, sensitivity, and strength help doctors decide the next steps to correctly diagnose the pain. Your medical history, pain levels, and previous treatments are discussed with your doctor to help them define the pain and decide on a treatment method.
Having tests like CT scans, MRIs, and X-Rays help doctors take an inside look at your pain. The images don’t always show the root cause of the pain, making FBSS hard to diagnose.
Since imaging is not always reliable, doctors may use another form of testing to diagnose your pain. This is called an aware state surgical examination. A doctor uses a small probe and stimulates the spinal cord, mimicking the pain, and triggering a response from the patient. This informs the doctor what type of pain the patient has and how it is caused.
Back pain patients are referred to pain management specialists who treat their pain and help improve their quality of life through short-term techniques.
Conservative Treatments for Failed Back Surgery Syndrome
There are many conservative treatments for FBSS.Besides the physical therapy and pharmacological therapy with over the counter or prescription medications, doctors use minimally invasive interventional modalities such as epidural steroid injections and injections of the lumbar facet joints or associated medial branches, with or without radiofrequency ablation rhizotomy (RFA).What makes these a consrvative first choice option is the minimally invasive nature of the procedures.These therapeutic interventions are designed to treat the pain and provide temporary symptomatic relief.
Neuromodulation in the Treatment of FBSS
In the treatment of Failed Back Surgery Syndrome, one of the most successful treatment options is Spinal Cord Stimulation. Treatment efficacy for FBSS has increased over the years with the majority of patients experiencing pain relief and reduced medicinal load. Improved quality of life can also be achieved using SCS.
For patients with unrelenting back pain due to mechanical instability of the spine, degenerative disc disease, spinal injury, or deformity, spinal surgery is a well-accepted treatment option; however, even after surgical intervention, many patients continue to experience chronic back pain that can be notoriously difficult to treat. Clinical evidence suggests that for patients with FBSS, repeated surgery will not likely offer relief. Additionally, evidence suggests long-term use of opioid pain medications is not effective in this population, likely presents additional complications, and requires strict management.
SCS has been shown to be a safe and efficacious treatment for this patient population. Recent technological developments in SCS offer even greater pain relief to patients’ refractory to other treatment options, allowing patients to regain functionality and improve their quality of life with significant reductions in pain.
To learn more about FBSS and how the team at Progressive Pain Management can help treat your pain, fill out the form below.
Facet joints are small, bony joints that sit along the spine. They are paired up from the neck to the lower back area. When the joints get inflamed, they cause pain that can be severe. The pain can be acute or chronic, caused by a variety of conditions.
The pain radiates to other parts of the body and causes indirect pain. For pain that starts in the lower back, it’s common for the pain to move to the thighs and buttocks. If the pain starts in the neck or upper back region, it can transfer to the shoulders, and arms, and even cause headaches.
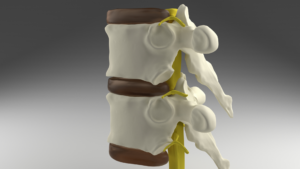
Facet Joint Injections for Chronic Pain
What is a Facet Joint Injection?
The injection is a strong anti-inflammatory steroid that gets inserted into the facet joint. The medication is a mixture of a local anesthetic and a steroid, similar to a cortisone injection. Before performing the injection, your doctor will explain the procedure, have you sign all the appropriate consent forms, and then have you lie on your stomach.
The procedure is minimally invasive. X-ray guidance is used to locate the facet joints and helps guide the needle to the exact location. The actual injection only takes a few minutes, but you may want to allow for additional recovery time depending on the type of anesthetic you choose. Some doctors will let you choose a local anesthetic or a stronger general anesthetic. The general anesthetic may cause drowsiness and sedation will take longer to wear off.
What to Expect After the Injection?
Right after the injection, you will feel relief from pain. That is due to the anesthetic in the injection, and only lasts for a few hours. The injection site may become sore after a few days, and the pain is not uncommon to resume the day after the injection. About 1-2 days after the injection, the medication will begin to take effect and help reduce your pain on a daily basis.
It is advised to take it easy following the injection and only to resume normal activity when it is comfortable to do so. Your doctor may recommend applying ice to the injection site. This will help reduce any swelling and soreness following the procedure.
How Long Does a Facet Joint Injection Last?
Immediately following the injection, you may feel lessened pain. However, this is temporary relief until the medication kicks in. That can take between 2-7 days after the injection.
If the first injection is successful in managing your pain, your doctor may perform additional injections. The amount of relief depends on your specific pain and because there are a variety of pain receptors in the spine, the long-term effect of these injections cannot be predicted. Everyone’s pain is different, so the treatment effectiveness will vary.
There are very few risks associated with this type of injection. The most common being tenderness and pain at the injection site, although this is temporary. Side effects of steroids may include weight gain, water retention, and temporary increase in blood sugar.
Facet joint injections are an excellent alternative to undergoing serious back surgery. Talk with your doctor today to discuss your options for getting relief from your pain and taking one step closer to bettering your quality of life.
Risks Associated with the Facet Joint Injection Procedure
As with any type of injection or invasive procedure, there are certain risks or complications that could arise:
- Allergies: In most cases, the allergic reaction is caused by the X-ray contrast or steroid, not the local anesthetic. Severe allergies are rare.
- Bleeding: In patients who are taking blood thinners or have a bleeding disorder, it is possible to have some bleeding as a result of the injection.
- Discomfort at the Injection Site: Worsened pain or discomfort at the injection site. Long-term pain is uncommon.
- Infection: Minor infections occur in less than 2% of facet joint injections. More complex infections are rare, only happening in 0.1% of injections.
Fill out the form below to contact the Progressive Pain Management team and learn more about facet joint injections.
Treating pain with hot and cold therapy can be very effective for a variety of conditions and injuries. This affordable, at-home therapy is often recommended to help relieve aches and pains from muscle or joint damage.
Heat therapy can utilize hot water bottles, heat pads, or warm baths. Cold therapy involves ice packs, cool water, or cold compresses. However, it can be confusing what type of aches and conditions call for hot therapy and which ones call for cold therapy. In some cases, using both may be a successful combination. Alternating heat and cold helps increase blood flow to the site of the pain.

Treating pain with heat and cold therapy
Cold Therapy
Cold therapy, also known as cryotherapy, helps reduce inflammation and swelling. It aids in slowing the rate of reducing tissue damage around a joint or tendon. Cold therapy can numb sore muscle tissue, almost acting as an anesthetic. It has the ability to slow down the pain signals that are transmitted to the brain.
Cold compresses are a common at-home treatment for standard injuries – RICE – Rest, ice, compression, elevation.
This treatment helps conditions such as osteoarthritis, injuries, gout, muscle strains, and tendinitis. It can also help reduce the pain induced by headaches or migraines.
Types of Cold Therapy
Cold therapy can be applied in a number of ways to an affected area. Common treatment options for at-home pain relief include:
- Ice packs: Cold compress or cold packs applied to an affected area for 20 minutes every 4-6 hours can reduce inflammation and swelling.
- Ice baths: Soaking in a cold (but not freezing) bath helps slow blood flow and reduce pain
- Coolant sprays
Other types of advanced cold therapy include:
- Using cold during stretching helps reduce muscle spasms. This is called try stretching.
- Cryokinetics combines active exercises and cold treatment to help ligament sprains.
- Whole-body cold therapy chambers
Heat Therapy
Heat therapy increases blood flow to a specific area and improves circulation. This is because heat on an inflamed area causes the blood vessels to dilate, promoting blood flow to the injured area. Applying heat to an affected area can provide comfort, increase muscle flexibility, and heal damaged tissue.
Improving circulation to a specific area is important in soothing discomfort and eliminating lactic acid waste that builds up after certain types of exercise.
Heat therapy is effective in treating chronic muscle pain or sore joints caused by arthritis, strains, and sprains, relieving pain or spasms due to neck or back injury, or tendonitis.
Types of Heat Therapy
There are two types of heat therapy: dry heat and moist heat. Regardless of the type of heat you choose, the heat should always be warm – not hot.
- Dry heat: This type of therapy includes heating pads, warm compresses, or hot water bottles. Dry heat is easily applied and simple to do at home.
- Moist heat: This version of heat therapy includes using steamed towels, warm baths (between 92 and 100 degrees Fahrenheit).
Moist heat often requires less application time and is considered to be more effective than dry heat. Professional heat therapies can also be utilized. This may include heat from an ultrasound, and is especially helpful when the pain is caused by tendonitis.
Minor stiffness and pain can often be relieved with 15-20 minutes of applied heat therapy.Heat should only be used no longer than 20 minutes at a time, up to three times a day, unless instructed otherwise by a medical professional.
Moderate-to-severe pain may be relieved by longer heat sessions, such as a soaking bath that lasts anywhere from 30 minutes to two hours.
Alternating Heat and Cold Therapy
In some cases, such as exercise-induced injuries, pain, or osteoarthritis, alternating between heat and cold therapy is most effective.
Cold therapy causes the blood vessels to contract and reduces circulation, decreasing pain. Removing the cold causes the veins to expand, increasing circulation. Heat therapy can assist circulation and the incoming flow of nutrients that can heal the injured tissues.
Contact the team at Progressive Pain Management to learn more about heat and cold therapy and how it can help temporarily relieve chronic pain.
Headaches are a common occurrence in adults. So much so that they are the most frequent complaint doctors hear from their patients. Headaches can be truly painful and debilitating from time to time, but are typically treated with over-the-counter NSAIDs or rest. However, in some cases, headaches can become so severe that medical attention is necessary.
It is important to understand the kind of headache you are experiencing and to know when to seek a doctor’s medical help.
The International Classification of Headache Disorders defines over 100 different types of headaches. Some headaches are caused by underlying conditions (secondary headaches) while others are the main medical concern. Those are called primary headaches, and there are three main types of primary headaches that cause people to seek the help of a doctor.

Types of Headaches
Three Most Common Types of Primary Headaches
Tension Headache
Tension headaches are the most common type of headache – 3 out of 4 adults experience this type of headache. Generally, tension headaches cause a dull pain on both sides of their head, sometimes with a squeezing pressure like your head is in a vice. The pain is usually mild-to-moderate, lasting anywhere between 20 minutes and 2 hours.
Stress and muscle tension, as well as genetics and environment are thought to cause these headaches. Fatigue is also thought to play a role.
Tension headaches are typically treated with over-the-counter medications like acetaminophen (Tylenol) or NSAIDs like aspirin (Aleve) or ibuprofen (Motrin). Always follow the directions on the label as misuse could result in severe side effects to your internal organs. If your headache is mild, a snack or short rest may help.
Migraine
Migraines are less common than tension headaches, but the symptoms are much more severe and intense. This throbbing pain is frequently accompanied by nausea, light sensitivity, and lack of appetite.
Women are 2-3 times more likely to suffer from migraines than men. Neurologists believe that migraines are caused by changes of blood flow to the brain and nerve cell activity, with genetics playing a large role. Many people who experience migraines have one or more family member with the same condition.
Migraines often come without warning and is commonly set off by a trigger. These triggers can vary from person to person. Some common triggers are:
- Changes in weather and humidity
- Fatigue
- Emotional stress
- Sensory triggers like flickering lights, strong smells, or loud noises
- Dietary triggers: chocolate, red wine, MSG, change in caffeine intake
Treatment for migraine headaches depends on the severity of your pain and frequency of this type of headache. Most migraines can be dissolved with over-the-counter medication. Although, if they become severe enough and are debilitating, doctors may prescribe medication for immediate relief, as well as a preventative drug to ward off future migraines.
Cluster Headaches
Cluster headaches are uncommon, but cause sudden onset severe pain that is felt behind the eyes. These headaches are much more severe than tension headaches or migraines and last between 1 to 3 hours. The pain may cause your eyes to become red and watery and eyelids may droop. Nausea may accompany the pain.
They are called cluster headaches because they come in clusters: a person can experience 1-8 headaches a day during a 2-month period every year or so. They typically occur at the same time of year with the pain being the same.
Unlike migraines, cluster headaches are 5 times more common in men than women. While there is no direct cause, they are frequently triggered by alcohol or tobacco use, foods that contain nitrates, or bright light. Certain lifestyle changes are recommended to reduce symptoms and the chances of having onset cluster headaches:
- Quitting smoking
- Prednisone; medication to reduce inflammation or swelling
- Diet changes – limiting food that is high in nitrates like lunch meat or bacon
- Limited alcohol
If those changes do not seem to improve your cluster headaches, doctors may prescribe medications such as lidocaine nose drops, verapamil, or sumatriptan. These drugs are often administered by injection.
If you suffer from any type of headache frequently, you should see a doctor. Frequent, constant headaches may be a sign of an underlying medical condition or lifestyle choice. It is important to work with your doctor and communicate your pain levels and symptoms with your physician so an effective treatment plan can be created.
Oops! We could not locate your form.

