Living with chronic pain is often associated with a decreased quality of life, and diminished state of mind and can put a lot of stress on one’s mental health. When your body aches, you know the pain is just not “in your head,” and the discomfort is real. Pain becomes your whole world.
Frequently, patients consider conventional ways of thinking: reducing activities and resting will reduce pain. However, the opposite typically occurs. When you reduce movement and daily activities, your body automatically reduces its capacity to function properly. This change in behavior leads to negative thoughts about pain – “will I ever be pain-free?” or “nothing helps my pain.”
This type of negative thinking affects other aspects of your life, leading to anxiety and depression. That is when therapies like Cognitive Behavioral Therapy are helpful.

Cognitive Behavioral Therapy for Chronic Pain
What is Cognitive Behavioral Therapy?
Cognitive behavioral therapy (CBT) is a form of talk therapy. It has been researched and proven effective across a myriad of diagnosed conditions. It helps people identify and develop skills to change negative thoughts and behavior. CBT is problem-focused and challenges the negative thoughts, beliefs, or concerns contributing to a patient’s mental health regarding their pain. It is more than a stereotypical therapy session that involves talking through a problem and focuses on “doing” things.
The science behind CBT says that individuals – not events or external stimulants – create their own experiences. This includes pain. People can train themselves to incorporate coping skills into their daily lives by changing awareness of pain and thought patterns. For patients with chronic pain, CBT helps patients break their pain cycles and improve their quality of life.
How is it used to Treat Chronic Pain?
Used to treat chronic pain, CBT is commonly used with other modalities of pain management. This may include massage therapy, medications, or physical therapy. CBT has minimal risk and side effects than medication or in extreme cases, surgery, making it an excellent treatment option.
Cognitive behavioral therapy can change a physical response in the brain that worsens pain. Pain causes stress which in turn affects the pain chemicals in the brain. CBT reduces the activity of those chemicals, making the body’s natural pain relief more effective.
The first step of CBT is education. When patients understand their diagnosis and how CBT can help, setting goals and getting in the correct mindset is easier. It also helps the patient identify triggers and behaviors that worsen their pain levels and allows them to learn adaptive behavior. The goal is to increase self-efficacy for managing and reducing chronic pain by correcting negative thoughts and beliefs. Cognitive behavioral therapy treats conditions caused by chronic pain, such as depression, anxiety, sleep disorders, and isolation.
What to Expect from CBT Sessions
CBT sessions vary depending on your provider and pain level, but the initial meeting may be used to normalize the patient’s experience. This involves normalizing their pain – they are not “crazy” or wrong for feeling their pain sensations. The pain is not “all in their head,” and they do not see a “shrink.” These are common concerns and worries of patients who suffer from chronic pain conditions.
There will be a clinical interview where patients are screened through a series of questions, self-reporting, and observations. This allows the doctor to provide feedback about their situation and allows them to educate them about how CBT can be used to help manage pain.
Paper material that use visuals to show the relationship of chronic pain and how it impacts feelings, behavior, thoughts, and their cycle of pain. When patients are able to understand and see these connections, it is easier to relate it to their lives. Visual materials also provide patients with assistance at home, promoting self-efficacy.
Cognitive behavioral therapy aids patients’ development of their own behavior. It “trains” them how to think, act, and feel regarding their pain. The sessions focus on teaching the importance of paced activities that increase function without overexerting yourself and how inactivity can worsen your pain. This trained development allows the patient to create specific, relevant, and achievable goals for themselves. It is often called SMART Goals: Specific, Measurable, Achievable, Relevant, Time-Limited goals.
By slowly incorporating activities into your daily routine, it takes away from the mindset of “My pain limits me” or “I can’t do this.” Once a mindset shift has been activated, any negative mood symptoms begin to dissolve.
CBT is often part of a comprehensive treatment plan, used in conjunction with interventional pain management techniques. The team at Progressive Pain Management works with your other healthcare providers to ensure you get the most out of your treatment plan and the highest quality of care possible.
Fill out the form below to get in touch with our team today!
Phantom limb pain is the sensation of pain that feels like it is coming from a body part that is no longer there. Once believed to be a psychological problem, research shows that phantom limb pain is a real sensation. The sensation originates in the spinal cord and brain.
What is Phantom Limb Pain?
Phantom limb pain is pain in an area with an amputation. The pain can be minor and go away on its own with the symptoms decreasing over time. However, phantom limb pain can be extremely debilitating and can lead to chronic pain. When the pain is consistent and continual for more than 6 months, the chances of your phantom limb pain disappearing on its own is slim-to-none.

The pain is real and not just a psychological phenomenon. During MRI scans, areas of the brain that were previously connected to the nerves in the amputated limb show activity when the patient feel pain.
What Causes Phantom Limb Pain?
The underlying root cause of phantom limb pain is not clear, but it originates in the spinal cord and brain. This is believed to be caused by a mixed signal in the brain. After amputation occurs, spinal cord and brain areas miss input sensations from where the limb should be. The body takes time to adjust. However, this lack of input sensations triggers the body’s most basic message that something is wrong: PAIN.
There are studies that show how, after an amputation, the brain “rewires” that part of the body’s sensory nerves to another part of the body. Because that amputated area is unable to receive sensory information, the information is referred. This means instead of feeling pain in the now-amputated leg, you feel those senses in a still-present hand.
Damaged nerve endings and scar tissue at the amputation site contribute to phantom limb pain. Sometimes the physical memory of the limb can invoke pain, as that sensory information has been retained.
Treatment Options
Treatment options vary depending on the severity of the pain sensations. Like many pain conditions, a combination of multiple treatment options is most effective in reducing pain. It can be difficult to treat phantom limb pain, but your doctor may begin with medication options and noninvasive treatments.
Some medications administered and prescribed to help phantom limb pain are as follows:
- Over-the-Counter Medications: Acetaminophen, Ibuprofen, or Naproxen may relieve phantom limb pain. These should be taken under the direction of your doctor.
- N-Methly-D-Aspartate (NMDA) Receptor Antagonists: This type of anesthetics bind to the NMDA receptors on the brain and blocks activity of glutamate – a protein that plays a crucial role in relaying nerve signals.
- Antidepressants: Tricyclic antidepressants may relieve the pain caused by damaged nerves.
- Anticonvulsants: Typically used to treat epilepsy, this medication is also used to treat nerve pain.
Other medications may include beta-blockers, sodium channel blockers and even low-dose narcotics if the pain is severe. Many physicians do not recommend taking narcotics and find other methods of relieving pain.
Noninvasive therapies do not always work for everyone, and just like medication, the effectiveness is monitored and measured in order to find the most viable solution to treat pain. Treatment options may involve:
- Acupunture: Acupuncture has been found to ease chronic pain symptoms. Long, fine, sterile needles are injected into pain points on the body, relieving tension and pain. It is an incredibly safe treatment option.
- Spinal Cord Stimulation: Tiny electrodes are placed along your spinal cord and an electrical current is delivered to the spinal cord and relieves pain.
- Heat Therapy
- Biofeedback: Training the body to effectively handle and manage pain by learning what the sensations feel like.
- Relaxation Techniques: Meditation, yoga, breathing techniques, and other methods of self-taught relaxation help you learn how to focus your energy away from the pain.
- Physical Therapy: Physical therapists design a treatment plan to incorporate cardio and strengthening exercises into your daily routine that help reduce pain and teach your body how to positively cope with pain.
If those options do not provide effective relief, surgery is available. Talk to your doctor today about starting a treatment plan if you suffer from phantom limb pain. The experts at Progressive Pain Management can help you manage your pain. Fill out the form below to get started.
When you are affected by pain, daily life, normal activities, and hobbies can become a challenge. Even the amount of sleep you get, the thoughts you have, and basic daily tasks can be negatively affected by pain.
Your quality of life and desire to resume regular activities plays an important role in maintaining your health and managing your pain. There are some positive changes you can make to your lifestyle and simple changes to your daily life that make managing your pain easy.

Tips for Living with Chronic Pain
Lifestyle Changes that Make Living With Chronic Pain Easier
Staying Active
Exercise can help those in pain find the relief they are looking for. Cardio exercise utilizes large groups of muscles and raises your heart rate. This combination releases endorphins. Endorphins are your body’s natural opiate (painkiller). Studies show that exercising for 30-45 minutes of low-intensity aerobic exercise is recommended and can help reduce pain.
Be sure to talk to a doctor before beginning any new exercise program.
A Good Night’s Sleep
Pain interferes with sleep – that’s a no brainer. When you are in pain, you are unable to achieve proper REM cycles and relax enough to get uninterrupted sleep. Pain can cause issues when falling asleep or staying asleep throughout the night.
Certain medications can also cause problems with sleep. If your medication causes drowsiness and fatigue, you may be more inclined to sleep during the day which can mess with your sleep at night. Getting the right amount of sleep at night is crucial to how your body copes with pain and how your body harnesses its energy levels.
Here are some ways to sleep better:
- Stick to a Routine: Creating a sleep routine can help you sleep better. Going to bed at the same time and setting an alarm for the same time every day can help train your body to get more meaningful rest.
- Watch What You Eat and Drink: Certain beverages – such as alcohol or caffeine – can affect your sleep patterns. Heavy meals have the same affect. If you have a snack before bed, eating something healthy like almond butter on toast, crackers and cheese, or nuts and fruit are great alternatives.
- Relaxation: Practicing relaxation techniques before bed can help get your mind and body prepared for a restful sleep. Try things like listening to soothing music, practicing deep breathing, and writing in a journal.
Reduce Stress Factors
Stress and pain go hand-in-hand. Your body may react in different ways when there is stress involved, such as tense muscles or headaches. This can be avoided by reducing stressors and managing stress levels.
Stress can cause negative impacts on your work ethic, eating habits, mood, and relationships. By keeping track of what stresses you out and considering how it affects your life. By eliminating or minimizing the stressors in your life, you may find ways to make your days or weeks go smoother.
Taking your life back from the pain caused by chronic diseases can be solved by adjusting your routine and activities. Contact the team at Progressive Pain Management to learn how to manage your chronic pain. Use the form below to get started.
What is Spinal Stenosis?
The spine consists of bones called vertebrae. The job of these bones is to provide stability and support for the upper body. Nerves run through the openings in the vertebrae and transmit signals from the brain to the rest of the body. If the surrounding bones or tissues get damaged, it can affect basic movements like walking, balance, and sensation.
Spinal stenosis is a condition that causes the spinal column to narrow and compresses the spinal cord. This does not happen quickly, but is a more gradual concern. Too much narrowing compresses the nerves in the spinal and causes problems.
While aging is the most common cause of spinal stenosis, conditions like osteoarthritis and rheumatoid arthritis can contribute to the pressure on your spinal cord.
How is Spinal Stenosis Diagnosed?
What are the Symptoms?
Symptoms can vary depending on the location of the stenosis and the nerves that are affected. Since spinal stenosis is a gradual onset condition, the symptoms tend to start slowly and worsen over time. In fact, spinal stenosis may appear on an MRI or a CT scan without the patient having any symptoms at all.
Cervical Spine
- Numbness or tingling in the hand, arm, foot, or leg
- Difficulty walking or with balance
- Neck pain
- Bowel or bladder conditions such as urinary urgency or incontinence
Lumbar Spine
- Weakness in the foot or leg
- Pain or cramping in one or both legs after long periods of standing or walking
- Back pain
- Numbness or tingling in the leg or foot
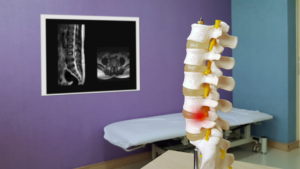
How is Spinal Stenosis Diagnosed?
Your doctor will diagnose spinal stenosis by reviewing your medical history and perform a physical examination. They will also want to discuss any symptoms you experience. After a full review, your doctor may order several imaging tests to pinpoint the cause of symptoms and signs.
Imaging tests may include:
X-Rays
X-rays can determine if there was a bone change that could affect the spinal column, such as bone spurs.
Magnetic Resonance Imaging (MRI)
MRIs utilize a powerful magnet and cross-sectional radio waves to produce images of your spine. MRIs detect issues with ligaments and discs. It also has the ability to determine if there is a tumor pressing on the nerves. The most important reason why MRIs are helpful is that they are able to show where the nerves in the spinal cord are being compressed.
CT Scan
If you are unable to have an MRI, a CT scan may be used instead. This type of imaging test combines X-Ray images that are taken at many different angles to create a detailed, cross-sectional image of your body.
Get started on getting the relief you deserve by fill out the form below. The team at Progressive Pain Management is here to help you reduce pain and enhance your quality of life.

