Migraines aren’t just a typical headache. Chronic migraines can wreak havoc on a person’s life. If you’ve experienced these extreme episodes, you know they are very painful and can have someone disabled for very long periods of time. Chronic migraines are a very real challenge, but thankfully, some things can be done to treat them.

Chronic Migraine Causes and Treatments
What is a migraine, and what causes it?
A migraine is a type of headache characterized by recurrent attacks of moderate to severe head pain that is often accompanied by nausea, vomiting, and sensitivity to light or sound.
Migraine headaches are believed to be caused by the dilation and contraction of blood vessels around the brain.
Migraines can be caused by factors such as dehydration, stress, or withdrawal from caffeine.
Medical experts are still unsure of the exact causes, but the consensus is a temporary abnormal brain function and misfiring of nerves.
Medical Treatment Options for Severe and Chronic Migraines
The two most common treatments for severe and chronic migraine are Botox and nerve blocks.
Botox is a procedure where injections of purified botulinum toxin are made into the muscle tissue of the forehead to reduce the muscle contractions in this region, which can lead to headaches.
Nerve blocks work by injecting pain medication (such as anesthetic or cortisone) around certain nerves in the neck, head, or face.
Holistic remedies include treatments such as acupuncture and biofeedback.
For more information on medications, remedies, and medical treatments, click here.
What Medicines are Available for treatment?
Anti-seizure medicines, along with beta-blockers and anti-depressants, are all within the realm of choices doctors go to to find treatments for their patient’s pain. Some aren’t advisable for pregnant women, or women who are attempting pregnancy, so keep that in mind!
How can Chronic Migraines be Prevented?
Depending on why they occur, chronic migraines can sometimes be prevented by certain lifestyle changes, such as drinking more water, working out, and eating better. But, sometimes, the causes are more complex than that, and prevention requires medical intervention. Those preventative measures can come in many forms, such as Botox, Calcium blockers, and certain supplements.
One typical supplement used to prevent migraines is magnesium. Magnesium interacts with the chemicals in the brain and can stop a migraine before it happens. For more information on using magnesium to treat chronic migraines, click here.
What will Happen During an Appointment to Find Treatment?
A specialist will sit with you and ask a range of questions surrounding your family history, genetics, and lifestyle. If further testing is needed, an MRI or CT scan may be needed, and then from there, treatment will be decided based on input from yourself and your doctor.
Migraines don’t have to take over your life; you don’t have to wait out the pain. Take control of your pain management and contact Progressive Pain Management to gather more information on how we can help you on your journey to a pain-free life!
Do you or a loved one experience chronic pain, limited mobility, and decreased quality of life even after undergoing back surgery? If so, there may be a condition called Failed Back Surgery Syndrome (FBSS) at play. FBSS is a common complication for people who have undergone various types of spine surgery for various spinal disorders.
While this difficult-to-treat syndrome typically occurs after lumbar spine surgery, it can also occur in the cervical and thoracic regions as well. Read on as we analyze the causes, symptoms, diagnosis, and treatment approaches available for patients affected by FBSS to help clarify this frustrating condition.
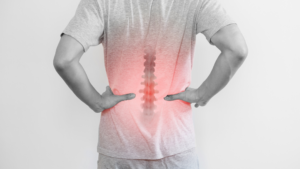
Failed Back Surgery Syndrome
fWhat is Failed Back Surgery Syndrome?
Failed back surgery syndrome occurs when patients experience persistent pain after undergoing spinal surgery. This pain can range from mild to severe and can be located in the same area where the pre-existing pain was before the surgery or even in an entirely new area. It is estimated that between 7% and 27% of all spinal surgeries result in failed back surgery syndrome.
Symptoms of Failed Back Surgery Syndrome
The symptoms of FBSS can vary widely, depending on the severity and location of the pain. Commonly reported symptoms include:
- Persistent back or leg pain
- Limited mobility or difficulty walking
- Numbness in the feet or legs
- Problems with bladder or bowel control
What Causes FBSS?
Failed back surgery syndrome can occur due to a variety of reasons, including scar tissue formation around the surgical site, nerve damage caused by the surgery itself, or undiagnosed underlying conditions that were not addressed during the original operation. Whatever the cause may be, it is essential to know that there are treatment options available to help manage your symptoms and reduce your pain.
Diagnosing Failed Back Surgery Syndrome
To diagnose FBSS, your doctor will ask about the history of your back pain and take a physical examination to assess any spinal instability. They may also use imaging studies such as an x-ray, CAT scan, or MRI to get an idea of what is going on in the spine. Other tests, such as an electromyogram (EMG) or nerve conduction study, may be done to measure how well your nerves are working.
Treatment Options for Failed Back Surgery Syndrome
There are several treatment options available for those suffering from FBSS, including:
- Physical Therapy – Physical therapy is often recommended as one of the first steps in treating FBSS. It focuses on strengthening weak muscles, increasing flexibility, improving posture, and teaching proper body mechanics to help reduce pain levels over time.
- Medication – Your doctor may prescribe pain medications as part of your treatment plan for FBSS, including non-steroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, or opioid medications such as oxycodone or hydrocodone. Your doctor will determine which medication(s) best suits your individual needs.
- Psychological Therapy – Cognitive behavioral therapy (CBT) is beneficial in treating chronic pain conditions such as FBSS. CBT helps patients develop healthy coping skills to deal with their pain more effectively and learn how to better manage stress levels.
- Spinal Cord Stimulation – Spinal cord stimulation (SCS) involves using electrical signals delivered through implanted electrodes placed near nerves within the spinal cord that have been identified as being involved with the patient’s chronic pain condition. SCS works by blocking or decreasing nerve signals associated with pain from reaching the brain.
- Alternative Treatments: In addition to traditional treatments such as medications and physical therapy, alternative treatments may be useful in treating FBSS symptoms. These include acupuncture, chiropractic care, yoga/meditation techniques, biofeedback training (a technique used to teach the body how to control its responses), and hypnosis techniques (which may help patients learn how to better cope with their chronic pain). While these alternative treatments cannot completely cure FBSS, they may provide additional relief when combined with traditional treatments like medications or physical therapy.
Get the Help you Need!
Failed back surgery syndrome (FBSS) is a very real phenomenon that can happen to anyone who has had spine surgery. FBSS often leads to chronic pain and can be extremely difficult to manage. If you or someone you love is struggling with FBSS, know that help is available. At Progressive Pain Management, we specialize in treating patients with FBSS and other complex cases of chronic pain.
We offer a wide range of treatments, from medication management to interventional procedures, and our team will work with you to create a customized treatment plan that fits your needs. Please fill out the form below to contact us today to learn more about how we can help you find relief from your chronic pain.
Arm and shoulder pain can be uncomfortable, inconvenient, and have a significant hindrance on everyday life if it goes without treatment. Sometimes the cause of arm and shoulder pain may be identifiable, resulting from a dislocation, separation, or prior injury. But sometimes, the cause of this pain can be a result of an underlying condition such as arthritis, tendonitis, or even gallbladder trouble. Regardless of the cause, many options are available to patients to treat arm and shoulder pain. Below is a list of some causes, non-invasive, and minimally invasive treatment options for those experiencing arm and shoulder pain.
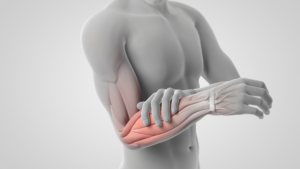
How to Treat Arm and Shoulder Pain
Causes of Arm and Shoulder Pain
It goes without saying that accidents can cause a variety of injuries to the arm and shoulder. Some of these commonly seen injuries include…
- Brachial Plexus Injury-Usually resulting from sports, auto, or motorcycle accidents, brachial plexus injuries occur when the nerves that send signals from the spinal cord to the arm and shoulder are compressed, stretched, or torn. Symptoms include numbness down the arm, weakness, and lack of arm movement.
- Dislocation-dislocation of the shoulder or elbow is an obvious form of injury that occurs when the joint is forced out of alignment or overextended. Distortion of the joint along with pain is a clear identifier of a dislocation.
Arm and Shoulder pain can also be caused by various pain conditions, including, but not limited to:
- Bursitis-Commonly known as joint inflammation, bursitis affects the fluid-filled sacs also known as bursae’s that cushion the bone, muscle, and tendon surrounding a joint. The shoulder, elbow, and hip are the most common areas where patients experience bursitis.
- Tendinitis-This specific inflammation of the tendon is commonly known as tennis elbow, golfer’s elbow, or pitcher’s shoulder. This is the irritation of the tendons that attach bone to muscle.
- Rheumatoid Arthritis-A chronic inflammatory disorder, rheumatoid arthritis is known for causing a painful swelling that affects the lining of joints. Tender, swollen joints, fatigue, and joint stiffness are common markers of this condition.
Treatments For Arm and Shoulder Pain
If you find yourself experiencing pain in your arm and/or shoulder, there are many treatment options available to you.
- Follow RICE measures…
- Rest-avoid strenuous activity and take a break from any movements that activate the pain
- Ice-apply ice for 15-20 minutes up to three times a day
- Compression-if necessary, use a compression bandage to help reduce swelling
- Elevation-elevate arm if possible to aid in reducing any swelling
- Take an anti-inflammatory such as Ibuprofen or Acetaminophen to help reduce pain and inflammation
- Corticosteroid injections are anti-inflammatory injections that your doctor can turn to for a more aggressive form of pain management
- Newer advancements in treatment suggest that the injection of NASHA hyaluronic acid is also effective in treating arm and shoulder pain, specifically in patients with osteoarthritis
It is important to note that severe arm and shoulder pain that comes on suddenly and is accompanied by fullness in your chest or any chest pain should receive immediate medical attention to rule out the cardiac arrest. However, the suggestions above should be considered as a first line of treatment for common forms of arm and shoulder pain. Of course, everyone responds differently to different types of treatment. If the pain does not go away or seems to worsen, contact your doctor and consider other forms of treatment. Depending on the cause, physical therapy or surgery may be necessary.
If you live with arm and shoulder pain, the team at Progressive Pain Management can help determine the root cause of pain and create a treatment plan. Fill out the form below to contact our team today!
If you’re suffering from chronic knee pain, you know that it can significantly limit your daily activities. Chronic knee pain can be debilitating and can prevent you from living your life to the fullest. From simple actions like taking a walk around your neighborhood to more strenuous duties like playing sports or running, an aching knee can keep you grounded.
But don’t give up hope! Understanding the underlying causes of chronic knee pain – and finding ways to alleviate it – is key to enjoying an active lifestyle. Also, there are many treatments available that can lessen and even possibly eliminate the debilitating effects of chronic knee pain. Read on to learn more about how these treatments can restore your life free from constant knee pain!

What is Chronic Knee Pain?
Chronic knee pain is classified as any pain in the knee that lasts three months or longer.
Symptoms
The symptoms vary from person to person and may include:
- Constant or intermittent pain
- Swelling and tenderness
- Loss of range of motion in the knee
- Redness and warmth around the affected area
- Stiffness
- Locking sensation
- Itching and burning
Causes of Chronic Knee Pain
The underlying causes of chronic knee pain can include:
Arthritis
Arthritis is the most common causes of chronic knee pain. Arthritis can refer to any condition that affects the joints, and it can range from mild discomfort to severe, debilitating pain. Osteoarthritis, also known as degenerative joint disease, is caused by excessive wear and tear on the cartilage between joints. Rheumatoid arthritis is another type that occurs when your immune system attacks your joints, causing swelling and damage to the cartilage and bones in your knees.
Tendonitis or Bursitis
Tendons are thick bands that connect muscles to bones in the body, while bursae are fluid-filled sacs that act as cushions between bones, muscles, and tendons. When these become inflamed due to injury or overuse, they can cause chronic knee pain. Tendonitis usually occurs when tendons become irritated due to repetitive use or overuse, while bursitis occurs when bursae become infected or irritated by nearby tissues.
Meniscus Tears
Your meniscus is a semicircular piece of cartilage located between your thighbone and shinbone inside your knee joint. A tear in this cartilage can occur due to trauma or age-related wear and tear, leading to sharp pains in the affected area. This type of injury often requires surgery if it does not heal on its own with rest and physical therapy.
How to Treat Chronic Knee Pain
There are several things you can do to improve your quality of life and reduce the severity of your chronic knee pain; these include:
Physical Therapy
Physical therapy is a great treatment for chronic knee pain that can help to improve mobility, reduce swelling and inflammation, and strengthen the muscles around the joint. Exercises such as stretching, strengthening, and range of motion exercises can be beneficial in relieving symptoms while also helping to prevent future injuries.
Over-the-Counter Medications
Over-the-counter medications such as nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to treat chronic knee pain by reducing inflammation and providing short-term pain relief. However, these medications should only be taken under a doctor’s supervision and may not be suitable for everyone.
Complementary Therapies
Complementary therapies such as acupuncture, massage, and yoga can all be beneficial in reducing chronic knee pain. These treatments can help to relax the muscles, improve circulation and reduce stiffness in the affected area.
Surgery
Surgery may be necessary when other treatments are ineffective in relieving chronic knee pain symptoms. Surgery typically repairs damaged ligaments or cartilage within the joint and may involve arthroscopy (a minimally invasive procedure) or open surgery (where larger incisions are required). Regardless of the type of surgery performed, it is important to follow a physical therapy program after surgery to ensure proper recovery and rehabilitation.
Rest and Relaxation
One of the best things you can do for yourself if you have chronic knee pain is to rest and relax as much as possible. This means avoiding activities that strain your knees or aggravate them further, such as running or jumping. Instead, focus on low-impact activities like walking, swimming, or biking. These types of activities will help strengthen the muscles around your knees without causing further damage or discomfort.
Long-Term Effects
Chronic knee pain can cause severe discomfort and negatively impact your quality of life. It is important to understand the long-term effects of chronic pain, such as:
- Loss of mobility
- Difficulty performing daily activities
- Depression
- Anxiety
Get Treatment for Your Knee Pain!
When it comes to treating chronic knee pain, there is no one-size-fits-all solution. Everyone’s pain levels and needs are unique, so finding the right combination of treatments to reduce your pain and improve your quality of life is essential.
If you’re suffering from chronic knee pain and want to learn more about what treatments are available, contact Progressive Pain Management and speak with a trained medical professional. We’ll work together to create a personalized plan that fits your lifestyle and works toward reducing your overall pain. To get started, fill out the form below to contact us today!
People have very different opinions on the cooler temperatures – either they love it, or dislike it. However, regardless of personal feelings, a degree drop affects the body similarly in everyone. A change in weather requires the body to function differently to conserve heat.
Those with chronic conditions and weakened systems can suffer, resulting in fatigue, worsened pain, and even immobilization. 92% of patients suffering from chronic pain believe their symptoms are exaggerated when the weather gets colder. Being aware of the impact of colder weather on your body can help reduce the pains of winter.

How Cooler Weather Can Affect Chronic Pain
Why A Drop in Temperature Results in Greater Pain
Despite a definitive, scientific relationship between cold weather patterns and chronic pain symptoms, patients report the changes their body experience when barometric pressure changes due to cold fronts and humidity changes.
Most of the reported pain symptoms result from swelling of joints and their surrounding tissues. When barometric pressure drops due to bad weather, the air pressure pushes with less force against joints. This allows the tissues to expand, which applies greater pressure to the joints. Patients with arthritis and fibromyalgia report aggravated pain.
Reduced temperatures can cause muscle stiffness, which makes moving and daily activities painful. However, remaining inactive leads to even greater pain. Spasms are more likely to occur when muscles are stiff and tight, leading to intense discomfort and pain. In patients with fibromyalgia, shortened muscles, caused by temperature drops in energy-deficient muscles is the main cause of pain.
For some patients, their chronic condition may be so severe that even a minor temperature change can result in worsened symptoms. It may be their first response to depend on a heating device, such as a heated blanket or hot water bottle. However, this can also cause painful side effects. Weakness, nausea, and changes in brain activity can result from overheating.
In patients who suffer from pain due to oversensitive nerves, the colder temperatures can cause widespread muscle and joint pain. An increase in nerve receptivity causes this. Cold weather negatively influences nerve conduction, so any pre-existing nerve damage becomes more noticeable.
Ways to Reduce Pain in Cooler Weather
Chronic pain patients can utilize a variety of methods to fight weather-related pain. Simple actions and changes to their daily lifestyle help keep the body warm and reduce pain caused by lower temperatures.
- Boost Your Vitamin D
Vitamin D is essential to maintaining energy and mindset. During the winter, it is common to battle seasonal depression and feeling slower due to reduced exposure to sunlight. Retaining higher levels of Vitamin D is important to help the body function properly and aids in reducing pain and stiffness. You can increase your Vitamin D intake by adding fatty fish and seafood to your diet, trying a UV light, or taking a supplement.
- Reduce Alcohol Intake
Winter alcoholic beverages may seem like they provide a cozy, toasty sensation, but they can actually lower body heat. Alcohol causes blood vessels to dilate, resulting in heat loss. Instead of having an alcoholic nightcap, try sipping on herbal tea to warm up and relax your body.
- Stay Active
Even if you can’t exercise outside, getting 30-45 minutes of cardio, strength, or flexibility training each day is recommended. Low-impact exercises such as yoga or tai chi help stretch the muscles and reduce mental stress. Cardio activities such as a treadmill or elliptical build muscle while increasing your heart rate.
It is important to remember to consult with your doctor before beginning any exercise routine. Even mild chronic pain conditions can be aggravated by overexertion. A physician can help determine appropriate exercises and stretches to combat your specific pain. Contact Progressive Pain Management by filling out the form below.

