Osteoarthritis is a gradual disease, with symptoms that appear over a long period of time. Depending on the joints and bones that are affected, symptoms vary, some that are more severe than others.
Osteoarthritis affects over 27 million Americans each year. The symptoms mirror those of other chronic illnesses as well as show up differently depending on the patient’s lifestyle, making it hard to diagnose. However, there are early signs of osteoarthritis to watch for that can help make an accurate diagnosis.
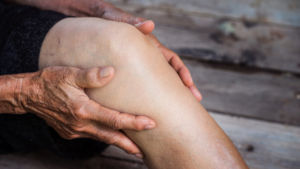
Osteroarthritis Warning Signs
Early Warning Signs of Osteoarthritis
- Joint Pain: Pain that worsens with activity and finds relief after a period of rest is suggestive of osteoarthritis. This is often one of the first signs of an issue with a joint. The discomfort of early osteoarthritis can be classified in two different ways: tenderness and pain. Patients don’t always suffer from debilitating pain, but experience aches or tenderness around the joints.
- Swelling: There is naturally occurring fluid in your joints. There is pain when the fluid builds up and causes the joint to swell. The extra fluid is created by the soft tissue that surrounds the joints.
- Loss of Flexibility: Early stages of osteoarthritis can cause body parts to not move as easily as before. Pain and stiffness contributes to this loss in flexibility and range of motion. Fully bending and extending a joint may become difficult or impossible. This has the ability to make daily activities hard to do. A loss in flexibility or range of motion is a very gradual process.
- Abnormal Sensations: The cartilage between your bones is meant to act as a “shock absorber” and to keep your joint moving smoothly. When this cartilage becomes worn out or torn, the bone-on-bone rubbing can cause abnormal sensations such as crackling, grating, or clicking can occur. Sometimes these sensations are felt, heard, or both. The bones rubbing together (grating) is common for patients with osteoarthritis.
- Joint Stiffness: Similar to joint pain, joint stiffness is commonly an early sign of osteoarthritis. Stiffness is common after sitting or laying for long periods of time. That sluggish, slow-to-move start in the morning could be an early sign of osteoarthritis. Oftentimes, joint stiffness fades as you move around and the joints have gotten a chance to loosen up.
If you experience these symptoms regularly, talk to your doctor. Test and examinations can be performed to accurately diagnose what is causing your pain. The earlier the detection, the more effective treatments will be. Osteoarthritis does not have a cure, but is manageable and there are treatments designed to help reduce pain and to help patients who suffer with pain get back to doing the things they love.
People who live with chronic joint pain know how debilitating it can be. Joint pain makes doing daily activities difficult and typically has a negative effect on the quality of life. It can steal away joy from doing the things they love and spending time with loved ones.
Chronic joint pain affects approximately 100 million Americans each year. Fortunately, there are exercises and self-care practices that help reduce and maintain pain. Exercises are designed to reduce inflammation, increase mobility, strengthen joints, and regain range of motion. Ideally, by implementing an exercise routine, there is no need for medication to manage the pain.
Working with a physical therapist or pain specialist is a great way to learn the proper exercise techniques that will help manage and reduce chronic pain. It’s important to remember not to force exercise or continue if it worsens your pain. Listen to you body and do what feels best!

Exercises to Help Reduce Chronic Joint Pain
Always consult your doctor before starting any exercise program.
Types of Exercises to Reduce Chronic Joint Pain
Stretching
Stretching helps relieve tension and stiffness that causes joint pain. Stretching does not require any equipment, so these can be done at-home, on-the-go, or even at work. Stretches are designed for certain areas of pain, like knee pain, neck pain, and back pain.
Cardio
Cardiovascular exercises have a large impact on chronic pain and reducing symptoms that are caused by living with pain. Little-to-no equipment is needed for cardio exercises and they are relatively easy to incorporate into your daily life. Walking is the easiest way to get moving and increase your heart rate, endurance, and strength. If walking is challenging at first, start with short walks and slowly build up the distance overtime.
Swimming and water aerobics are another great cardio option for those living with chronic pain. Being in the water takes the pressure off your joints so you can exercise with ease. This is especially important for patients with low-mobility. Moving in the water adds natural resistance while no additional stress or pressure on your joints is present. Being in the water is often therapeutic, too. Improving your mood is critical to managing chronic pain.
Low-Impact Group Classes
Low-impact exercises are a great way to build muscle strength to better support joints that cause pain. Group setting classes, such as cycling or aerobics, can be beneficial to pain patients. Group classes are usually designed around a certain level of ability, meaning pain patients can take classes that best suit their needs and functions. Group settings are also great for accountability, which is important when trying to exercise regularly.
Cycling, for example, is a smoother motion for the joints than jogging, which can cause further damage and pain. If your pain levels allow, trying cycling a few times a week. The pedaling motions and breathing rhythms are excellent for increasing oxygen flow to the muscles and releasing endorphins that reduce chronic pain.
Balance Exercises
Exercises that focus on balance, core strength, and self-awareness like Yoga, Tai Chi, and Pilates are excellent for managing pain. They improve coordination and balance, which helps increase a sense of where joints are located and how to relieve tensions and pressure on those joints. These exercises include moves that increase flexibility and range of motion. This can loosen joints, which improves their function.
These exercises will help teach proper posture and body positions that align your joints and muscles, in hopes that your pain will be reduced. At Progressive Pain Management, our team can help create a plan incorporating exercise with interventional pain management techniques.
Fill out the form below to learn more.
Lower extremity pain is commonly due to overuse and inflammation as a result of conditions that affect bones, joints, muscles, tendons, and other organs. The key to pain is understanding what causes it. Only physicians can truly diagnose this kind of pain. There are a few questions to ask when diagnosing pain in your legs, hips, thighs, ankles, and lower joints.
- Is there a recent trauma? Falls to the ground are a common cause for lower extremity pain. This is especially true when a patient is unable to recall periods of time or suffers from a drug withdrawal. There is a chance of fracture, so radiographs should be taken.
- Is the pain articular or non-articular? Articular pain (meaning joint pain) is often accompanied by inflammation or swelling. Non-articular pain is musculoskeletal pain and affects muscles and bones. These differentiating symptoms help physicians diagnose the potential source of the pain.
- What is the root of the pain? When determining and understanding the root of the pain, physicians consider a broad variety of symptoms and characteristics regarding your pain. Things like infection, inflammation, vascular, and neoplastic causes can disguise other sources of pain.
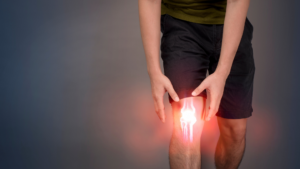
Being able to answer those questions helps pain doctors diagnose pain and recommend effective treatments for lower extremities. The term “lower extremities” includes the pelvis and hip joint, thigh, knee, lower leg, ankle, and feet.
Types of Lower Extremity Pain
Ankle
Because your ankle bears the weight of your entire body, it is prone to injury. The ankle is a complex network of bones, tendons, muscles, and ligaments. This means there are a lot of things that can cause pain.
Ankle pain can be caused by a number of conditions, including, but not limited to:
- Achillies tendonitis
- Gout
- Osteoarthritis
- Plantar Fasciitis
- Sprained Ankle
- Stress Fractures
Thigh
Pain in your thigh commonly starts in nerves that surround the hip and radiate down. Muscle pain, nerve pain, and injuries are all factors to consider when looking at thigh pain.
Pain may be caused by:
- Bernhardt-Roth syndrome
- Overuse
- Sciatica
- Peripheral Neuropathy
- Sprained or torn ligament
- Blood clots
Foot
Foot pain can be caused by overuse and conditions that cause inflammation like injury to tendons or ligaments in the foot. Arthritis is a common cause of foot pain. The bottom of the foot has a network of nerves that when damaged, cause immense burning sensations, numbness, or tingling.
Common causes of foot pain include:
- Osteoarthritis
- Mortnon’s Neuroma
- Plantar Fasciitis
- Gout
- Diabetic Neuropathy
- Tendonitis
Lower Leg
Leg pain can be caused by a wide variety of conditions and injuries. Generally, the leg pain is a cause of tissue inflammation. This can be a result of injury or chronic diseases. The leg contains many different types of tissues and bone structures, making injury and pain very common.
Leg pain can be caused by:
- Shin Splints
- Stress Fractures
- Diabetic Neuropathy
- Peripheral Artery Disease
- Sciatica
- Deep Vein Thrombosis
Hip and Pelvis
Hip and pelvis pain can be difficult to diagnose. The movement of the hip joint, lower back, and leg bones are all connected by a large network of muscles, ligaments, tendons, and joints. Pain from another area of the body frequently causes pain in the hip and pelvis region. This is called referred pain.
Sources of pain can include:
- Bone Fractures
- Arthritis
- Nerve Damage
- Muscle Injury or Inflammation
Knee Joint
If you use your knees to repetitively kneel or lift heavy objects, you may experience knee pain. Knee pain affects people of all ages. Injuries are common and regularly affect the ligaments, tendons, or fluid-filled sacs that surround the bone. Cartilage in the knee also gets damaged from normal wear and tear, which can cause pain.
Common causes for pain include:
- Osteoarthritis
- Meniscal Injuries
- Cysts
- Gout
- ACL tears
- Bursitis
Treatment Options
Once a diagnosis has been made, your physician will create a treatment plan specific to your pain. If the cause is musculoskeletal, non-steroidal medications or acetaminophen may be used. If pain persists, stronger medications may be prescribed, although it is rare that narcotics are needed.
If the pain is articular pain, corticosteroid injections may be used to reduce pain. Muscle and tendon pain can be reduced using physical therapy. However, if the muscle pain is due to arthritis, physical therapy may not be helpful.
Your doctor will work with you to create an effective treatment plan that fits your lifestyle and provides the greatest success in restoring a higher quality of life. The team at Progressive Pain Management can help diagnose the underlying cause of your lower extremity pain and find a relief solution. Fill out the form below to contact the team today.
The Dorsal Root Ganglion (DRG) is a small bundle of nerves connected to each vertebra along your spine. The DRG is critical in processing pain signals and transmitting them to your brain. They have a particularly important role in how you experience pain. The DRG act as the body’s internal traffic light: they control when signals can enter the spinal cord, therefore allowing pain signals to travel to the brain.
The Dorsal Root Ganglion neurons modify your sensory perception (how you feel pain) before transmitting the signal to your spinal cord and central nervous system. This makes DRG stimulation an effective treatment approach for patients with chronic pain.

What is Dorsal Root Ganglion Stimulation?
Dorsal Root Ganglion stimulation utilizes a pulse generator that is implanted on the spine. The implant uses small electrical leads which are threaded into the epidural space where the DRG lies. The leads send a small electrical impulse to the area where the DRG is located. The impulses stimulate the Dorsal Root Ganglion to create a “red light.” This blocks pain signals from that specific area traveling to the brain.
The impulses either create a slight tingling sensation in the affected area, or has the ability to stop the pain altogether.
Benefits of DRG Stimulation
There are four specific benefits of targeting the Dorsal Root Ganglion for pain relief:
- Directed Targeting: Because the stimulator is implanted exactly where the pain is rooted, DRG stimulation can relieve pain in a specific area. The accuracy of this treatment has proven effective in 94.5% of patients who received targeted areas of pain.
- Low Energy: DRG stimulators use a tiny amount of energy – only about 10% of the energy that is required from a conventional spinal cord stimulator. The batteries in the DRG stimulator last longer because of the low energy requirement.
- Low Risk of Lead Migration: The DRG stimulators are tucked into a small space, limiting the chances of lead migration. There is reported less than 1% migration rate, whereas a traditional SCS reports an approximate 14% migration rate.
- Minimal Effects on Body Position: Due to the DRG’s location in the epidural space, the cerebrospinal fluid in between electrodes does not affect the patient’s posture or body position. The stimulation patterns remain constant regardless of any changes in the body’s position. Whether lying down, sitting down, standing, or walking, the patient receives the same pattern.
Your physician will first implant a trial DRG Stimulator using fluoroscopic guidance. Data is collected from this and evaluated to determine whether or not a permanent stimulator is beneficial.
If you think you are a good candidate for DRG Stimulation, fill out the form below. Someone from our team will get in touch!
Sciatica causes pain to radiate along the sciatic nerve’s path. It can disturb daily activities, quality of life, and causes discomfort. Pain can be caused when the nerves get pinched, and intense pain can travel into your legs. Sciatica can be repetitive, intolerable, and many times, the cause is unknown to the patient.
This type of pain can be treated with self-care and rarely requires medicine. Treatments depend on what is causing the underlying root of the pain. Natural remedies are available and can dramatically improve a patient’s condition. Patients should always be discussed with a medical professional before beginning any type of treatment.
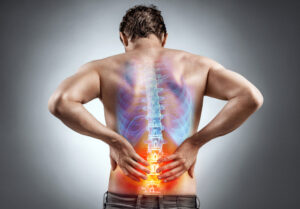
Natural remedies for sciatica
5 Natural Remedies for Sciatica Pain
Chiropractor
Patients who suffer from sciatic nerve pain often find relief from chiropractic adjustments. Adjustments can improve spinal function and in turn, reduce pain.
Yoga
While sometimes moving can aggravate sciatic pain, certain types of movements and stretching can actually reduce pain. Stretches that lengthen the spine or yoga positions that help develop good posture help reduce stiffness, inflammation, and pain.
Yoga is safe and effective for people with sciatic pain. It can strengthen core muscles, relax stiff areas, and help prevent further pain.
Acupuncture
Acupuncture is a traditional Chinese practice that maintains health by releasing the body’s natural energy. Tiny needles are injected into specific, targeted areas. Acupuncture helps improve blood flow, oxygen, and channels energy in a holistic approach. It has been FDA approved to treat back pain and chronic pain of all kinds, including sciatica.
Active Lifestyle
Working at a desk or lounging too long can worsen back pain. Sciatica treatments frequently recommend movement and staying active. An active lifestyle and targeted exercises allow for joints and affected areas to loosen up and relieve pain. Isometric exercises help relieve pain during the day; many of these can be performed at work or on the go. If you typically lead a somewhat sedentary lifestyle, investing in a fitness tracker can help motivate you to set activity goals.
Heating Pads
Heat loosens tight muscles and promotes blood circulation. Many people with sciatica find pain relief by using heating pads on a low setting for 15-20 minutes daily. Applying heat to the affected or painful area can be performed a few times a day, every few hours. Many heating pads are small and travel well, so it can be helpful to use while sitting at work. Another method of heat is taking warm baths. Water relieves pressure from your joints, also reducing pain, while the heat loosens up the muscles. For use on-the-go, one-time-use heating wraps may be used that are effective for several hours.
If you suffer from sciatica pain, the team at Progressive Pain Management can help. Fill out the form below to get in touch.

